Advertisement
Grab your lab coat. Let's get started
Welcome!
Welcome!
Create an account below to get 6 C&EN articles per month, receive newsletters and more - all free.
It seems this is your first time logging in online. Please enter the following information to continue.
As an ACS member you automatically get access to this site. All we need is few more details to create your reading experience.
Not you? Sign in with a different account.
Not you? Sign in with a different account.
ERROR 1
ERROR 1
ERROR 2
ERROR 2
ERROR 2
ERROR 2
ERROR 2
Password and Confirm password must match.
If you have an ACS member number, please enter it here so we can link this account to your membership. (optional)
ERROR 2
ACS values your privacy. By submitting your information, you are gaining access to C&EN and subscribing to our weekly newsletter. We use the information you provide to make your reading experience better, and we will never sell your data to third party members.
Pharmaceuticals
Nanochains Light Up Metastatic Cancer Cells
Medical Imaging: Particles’ oblong shape could help detect spreading tumors
by Sarah Webb
October 1, 2012

When a cancer metastasizes, oncologists struggle to find and treat the small clumps of cancer cells that pop up in other tissues. Now researchers have designed a chain of iron oxide nanoparticles that can highlight metastatic tumors in mice (ACS Nano, DOI: 10.1021/nn303833p).
Scientists would like to target nanoparticles to metastatic cancer cells as they do to normal cancer cells: They decorate the particles with a protein or small molecule that binds to proteins expressed at high levels on the surfaces of the cells. The particles then deliver drugs or serve as labels for imaging techniques, such as magnetic resonance imaging (MRI).
One possible particle decoration for metastatic cells could be short peptides that bind ανβ3 integrins. Cells in metastases, and in the newly formed blood vessels that feed them, express high levels of these integrin proteins on their membranes, says David Cheresh of the University of California, San Diego’s Moores Cancer Center. In a 2008 study, Cheresh and his colleagues showed that a lipid nanoparticle labeled with integrin-binding peptides and carrying chemotherapy drugs accumulated in newly formed blood vessels and inhibited metastasis (Proc. Natl. Acad. Sci., DOI: 10.1073/pnas.0803728105).
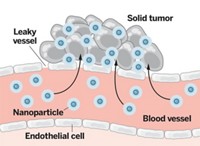
Efstathios Karathanasis and his colleagues at Case Western Reserve University thought that tweaking the shape of nanoparticles could further improve their ability to find metastatic cells. Nanoparticles are typically spherical because that is the easiest shape to make, says Karathanasis. In a fluid flow, such as the one found in blood vessels, spheres typically stay in the center. Meanwhile, oblong structures would more likely drift toward the edges of a blood vessel, he thought, where the integrin-coated cells reside. Also, compared to a sphere, says Karathanasis, a rod-like shape’s flatter surface would enable more of the particle’s peptides to interact with the surfaces of cells they bump into.
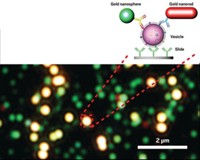
To make such an oblong particle, Karathanasis and his colleagues linked iron oxide nanospheres using a technique they published previously (PLoS ONE, DOI: 10.1371/journal.pone.0005843). The resulting nanochains contained on average four spheres and were 100 nm long. They then decorated those chains’ surfaces with integrin-binding peptides and a fluorescent label.
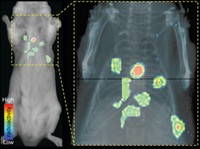
The team tested their particles as imaging agents in mice injected with a metastatic form of breast cancer. The fluorescent tags allowed the researchers to use a microscope to initially follow the particles’ movements toward tumors and metastases. Then the scientists placed the rodents in MRI machines to test whether their nanochains could highlight areas with metastases. Areas in the lungs and liver of the mice lit up in the MRI scans. They confirmed that these tissues contained metastases when they looked at slices of the tissue under a microscope.
To determine the diagnostic power of the particles, the team now wants to work out the percentage of small metastases in an animal that they can identify with the nanochains and MRI. They also need to study the particles’ toxicity, Karathanasis says.
Cheresh, who was not involved in the work, says that the study shows that optimizing particle shapes could improve the efficacy of particles targeted to cancer cells. Such targeting enhancements will be critical for treating patients with metastasizing cancers, he says.


Join the conversation
Contact the reporter
Submit a Letter to the Editor for publication
Engage with us on Twitter