Advertisement
Grab your lab coat. Let's get started
Welcome!
Welcome!
Create an account below to get 6 C&EN articles per month, receive newsletters and more - all free.
It seems this is your first time logging in online. Please enter the following information to continue.
As an ACS member you automatically get access to this site. All we need is few more details to create your reading experience.
Not you? Sign in with a different account.
Not you? Sign in with a different account.
ERROR 1
ERROR 1
ERROR 2
ERROR 2
ERROR 2
ERROR 2
ERROR 2
Password and Confirm password must match.
If you have an ACS member number, please enter it here so we can link this account to your membership. (optional)
ERROR 2
ACS values your privacy. By submitting your information, you are gaining access to C&EN and subscribing to our weekly newsletter. We use the information you provide to make your reading experience better, and we will never sell your data to third party members.
Diagnostics
Near-infrared dyes specifically light up nerve tissue
Probes could pave the way for fluorescence-image-guided surgery that spares nerves
by Celia Arnaud
April 2, 2019

Nerve tissue can be hard to spot during surgery. Hundreds of thousands of nerve injuries occur annually in the US when surgeons cut nerve tissue by mistake. To help surgeons better avoid nerves, researchers at the Oregon Health and Science University have made the first near-infrared (NIR) fluorophores that specifically bind to nerves.
Lei Wang, a postdoctoral fellow working with biomedical engineer Summer Gibbs, reported the findings Tuesday morning at the American Chemical Society national meeting in Orlando during a session in the Division of Analytical Chemistry.
Other nerve-specific fluorophores exist, but they get excited by and emit light in the visible spectrum. NIR probes are preferable for biological imaging because the light can penetrate deeper into tissue and background fluorescence from the tissue itself is at a minimum.
Wang and his colleagues designed and synthesized a library of 66 fluorophores based on an oxazine scaffold, starting from a known visible-light, nerve-specific fluorophore. Because what makes a fluorophore nerve-specific is poorly understood, shifting a fluorophore to NIR wavelengths while preserving its nerve specificity was challenging.
When Wang and his colleague Connor Barth, a research scientist in Gibbs’s group, screened the library, they found eight nerve-specific fluorophores with the desired NIR fluorescence. They are focusing on two of those fluorophores for further studies.
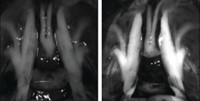
“Our two favorites give relatively bright nerve signals and high nerve-to-background-tissue ratios,” Gibbs told C&EN. One is fast acting, achieving high contrast within 15–20 min of intravenous administration in mice and pigs. The nerve-specific signal persists for about 3 h. The other fluorophore is longer acting, taking about 90 min to develop contrast but lasting for at least 6 h.
Surgeons already use image-guided systems to help them determine which tissue to cut and remove, and these systems work with fluorescence in the 700–800 nm range, with 800 nm being more widely used. “Basically all infrastructure in the fluorescence-guided-surgery space has the 800 nm channel designed around indocyanine green,” a dye currently used in medical diagnostics, Gibbs told C&EN. The team’s current best compounds are compatible with the 700 nm channel of clinical image-guided surgery systems.
To better match existing clinical image-guided surgery infrastructure, the team has already identified other chemical scaffolds that emit around 800 nm while maintaining nerve-specificity. Before those molecules can be used clinically, their fluorescent properties need further optimization.
Nerve-specific dyes would allow surgeons to improve nerve-sparing surgical procedures. Eric R. Henderson, an orthopedic surgeon at Dartmouth–Hitchcock Medical Center, told C&EN, “The ability to have special identification of nerve tissue, particularly in the setting of aberrant anatomy, would enhance the safety and efficacy of surgery and pave the road to machine recognition of nerve and other human tissues and eventually to robotic surgery.”
Gibbs’s team has demonstrated the nerve-specific NIR fluorophores in mice and pigs. They are currently pursuing additional studies that will be necessary for an Investigational New Drug application to the US Food and Drug Administration before human clinical trials.


Join the conversation
Contact the reporter
Submit a Letter to the Editor for publication
Engage with us on Twitter