Advertisement
Grab your lab coat. Let's get started
Welcome!
Welcome!
Create an account below to get 6 C&EN articles per month, receive newsletters and more - all free.
It seems this is your first time logging in online. Please enter the following information to continue.
As an ACS member you automatically get access to this site. All we need is few more details to create your reading experience.
Not you? Sign in with a different account.
Not you? Sign in with a different account.
ERROR 1
ERROR 1
ERROR 2
ERROR 2
ERROR 2
ERROR 2
ERROR 2
Password and Confirm password must match.
If you have an ACS member number, please enter it here so we can link this account to your membership. (optional)
ERROR 2
ACS values your privacy. By submitting your information, you are gaining access to C&EN and subscribing to our weekly newsletter. We use the information you provide to make your reading experience better, and we will never sell your data to third party members.
Environment
FDA Revisits Dental Amalgams
Agency weighs safety concerns related to mercury exposure
by Britt E. Erickson
January 31, 2011
| A version of this story appeared in
Volume 89, Issue 5
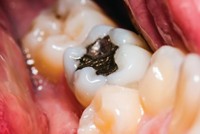
Used for more than 150 years to fill cavities and restore decayed teeth, dental amalgams, which are about 50% mercury and 50% silver, tin, and copper alloy, continue to spark debate over their safety. Not only is there a question about how much mercury escapes as volatile Hg(0) into the mouths of patients, but the best biomarker for measuring mercury exposure is also unclear.
These and other questions are at the heart of several petitions challenging a 2009 Food & Drug Administration regulation of “silver” dental fillings. As a result, the agency is taking another look at the safety of dental amalgams.
“Mercury in dental fillings is released as a vapor in low amounts that can be inhaled in the lungs and then absorbed by the blood,” Nancy Stade, deputy director for policy at FDA’s Center for Devices & Radiological Health, told reporters last month during a briefing in preparation for a two-day FDA advisory panel meeting on dental amalgams. “We know that exposure to high levels of mercury vapor can result in brain and kidney damage,” she added. The question facing regulators is whether the level of mercury released by amalgams requires a change in policy.
Dental amalgams are currently regulated under a rule finalized in 2009 that upgraded the material from a Class I medical device to a Class II device. The higher classification means that dental amalgams pose a greater risk to patients than previously thought, and special regulatory controls, including a guidance document for manufacturers, are needed.
Several antimercury advocacy groups, including the International Academy of Oral Medicine & Toxicology and Moms Against Mercury, as well as passionate victims of mercury poisoning and their families, believe FDA did not go far enough in its reclassification. Many of them petitioned FDA in 2009, and they came out in full force at last month’s panel meeting to urge the agency to ban dental amalgams or reclassify the material as a Class III medical device. Class III is the highest risk category for medical devices and, unlike other classes, requires extensive proof of safety.
The groups pressed FDA to immediately restrict the use of dental amalgams in susceptible subpopulations, such as children, pregnant women, and people who are genetically predisposed not to excrete mercury. Many victims representing those subpopulations provided the panel with compelling personal accounts of harm caused by dental mercury.
“It is time for FDA to turn aside from its mistaken policies about silver dental fillings, disclose the risks to consumers, and discontinue using mercury fillings in children and young women, and in particular pregnant women,” stressed Carol J. Ward, vice president of Dental Amalgam Mercury Solutions, a support group for individuals poisoned by dental mercury.
Last month’s FDA meeting brought together experts in risk assessment, toxicology, epidemiology, and dentistry. At the gathering, an FDA advisory panel heard about various biomarkers of mercury exposure, different ways to calculate a safe daily exposure level, and the strengths and weaknesses of existing clinical studies on dental amalgams.
In addition to addressing concerns about the levels of exposure to mercury vapor and the adequacy of FDA’s risk assessment used to classify dental amalgam, the meeting included discussion about the lack of information given to patients regarding mercury in dental amalgams.
Panel members acknowledged that some individuals are likely to be more prone to health effects from dental amalgams than others, but susceptible subpopulations are not easy to identify in advance, they said. Some panelists suggested adding new warnings to dental amalgam labels to make dentists more aware of sensitive groups.
The panel also spent a lot of time discussing which biomarker is best for estimating exposure to mercury from dental amalgams. “There are some arguments about what really should be the proper matrix to look at mercury,” G. Jean Harry, head of the neurotoxicology group at the National Institute of Environmental Health Sciences, told the panel. “Is it blood, urine, feces, hair, or nail?” she asked, adding that the answer will depend on the type of mercury being analyzed.
Harry also recommended that the panel think about whether concentrations change as a function of sampling time. “One component may be in the feces in the first 24 hours and in the urine later,” she said. She urged the panel to also consider whether exposure to mercury from dental amalgams is continuous, occurs in acute bursts, or is a combination of the two.
There seemed to be some consensus at the meeting that urinary mercury is a good biomarker for estimating exposure. “Urine is the best we have right now. When you compare urinary mercury concentrations with the number of dental amalgam fillings, you see a very strong relationship above a certain mercury level,” noted panel member Susan Griffin, a senior toxicologist with the Environmental Protection Agency’s Superfund program in Denver. “But when you get down to the very low mercury concentrations, that relationship seems to fall off.”
Anne O. Summers, a metallobiologist with the University of Georgia, presented the panel with results from animal studies that support the use of feces as a biomarker. The studies show that mercury from dental amalgams is methylated in the large intestine and excreted as methylmercury in feces.
That presentation raised the question of how to tease out the impact of other sources of mercury, such as methylmercury from eating fish. The panel also wrestled with how to handle risk assessments involving exposure to mixtures, such as when a person is exposed to high levels of a pesticide or lead in addition to mercury.
A lot of debate also took place over the best way to calculate a safe daily exposure level, often called the reference exposure level (REL), for mercury in dental amalgams. Several petitioners have argued that the REL for chronic mercury vapor exposure used by FDA is not protective enough. FDA relied on an REL of 0.3 μg Hg/m3 derived by EPA in 1995. Other government entities have used more protective uncertainty factors to derive lower RELs. For example, Health Canada has an REL of 0.06 μg Hg/m3, and California EPA has an REL of 0.03 μg Hg/m3.
Questions about the safety of alternatives to dental amalgams also came up during the meeting. For example, composite fillings contain bisphenol A, another controversial chemical known for its estrogen-like behavior. Panelists noted that amalgams are often better for multiple surface restorations and last longer than composite fillings.
Because of the complexity of the science, antimercury groups aren’t optimistic that FDA will change its dental amalgam regulation anytime soon. While they wait for FDA to make a decision, they are focusing their attention on a United Nations Environment Program global treaty (C&EN, March 2, 2009, page 13) that could phase out all uses of mercury. They see the treaty, which could be legally binding by 2013, as their best hope for banning dental amalgams in the U.S.
“FDA’s amalgam policy is particularly embarrassing as the U.S. enters negotiations for a world mercury treaty—a priority for the Obama Administration,” James S. Turner, attorney for petitioner Citizens for Health, emphasized at the meeting. “While all the other stakeholders—governments, nongovernment organizations, international bodies—are focused on eliminating mercury products, FDA is telling the world that mercury fillings are good for the public health.”




Join the conversation
Contact the reporter
Submit a Letter to the Editor for publication
Engage with us on Twitter