Advertisement
Grab your lab coat. Let's get started
Welcome!
Welcome!
Create an account below to get 6 C&EN articles per month, receive newsletters and more - all free.
It seems this is your first time logging in online. Please enter the following information to continue.
As an ACS member you automatically get access to this site. All we need is few more details to create your reading experience.
Not you? Sign in with a different account.
Not you? Sign in with a different account.
ERROR 1
ERROR 1
ERROR 2
ERROR 2
ERROR 2
ERROR 2
ERROR 2
Password and Confirm password must match.
If you have an ACS member number, please enter it here so we can link this account to your membership. (optional)
ERROR 2
ACS values your privacy. By submitting your information, you are gaining access to C&EN and subscribing to our weekly newsletter. We use the information you provide to make your reading experience better, and we will never sell your data to third party members.
Biological Chemistry
Fighting fungal infection with targeted therapy
Tweaking the structure of a membrane-disrupting antifungal compound reduces collateral damage to mammalian cells
by Erika Gebel Berg
February 23, 2017

Some antifungal medications can’t distinguish between a fungus and us, leading to potentially serious side effects. For certain systemic infections, amphotericin B (AmB) is the only effective antifungal agent available, but it’s also one of the most toxic drugs in clinical use since it indiscriminately ruptures membranes of both fungal and human cells. To make a more selective drug, researchers have now altered how AmB interacts with membranes, allowing it to weaken fungal membranes while leaving mammalian membranes intact (Bioconjugate Chem. 2016, DOI: 10.1021/acs.bioconjchem.6b00629). The approach may be generalizable to other membrane-disrupting medications, including many antibiotics.
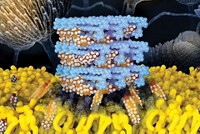
The exact mechanism for AmB’s activity isn’t known, but Steven L. Regen of Lehigh University and others have shown that the agent exists as either monomeric, individual molecules, or as aggregates. Monomeric AmB, he says, punctures the membrane surface to create a leaky cell that eventually dies, whereas the aggregate goes deep into the membrane and causes a catastrophic rupture that “blows the cell apart.” Importantly, the monomeric form selectively acts on fungal cells, he says, whereas the aggregate kills indiscriminately. Regen’s team wanted to “tame the aggregate,” blocking it from killing cells, while letting the monomeric form continue to target fungi.
To stop the aggregate from deeply penetrating cellular membranes, the researchers covalently linked AmB to a molecule of cholic acid. This bile acid is thought to align itself on top of membranes, so Regen’s team hypothesized that it could act as a chemical tether for AmB, keeping the aggregate from fully penetrating the membrane.
The researchers tested this using sheep red blood cells. When treated with AmB alone, even at low concentrations, these cells release all of their hemoglobin, an indicator of catastrophic rupture. But when the researchers added the AmB-cholic acid conjugate, the cells largely kept their hemoglobin inside. This held true at concentrations much higher than would typically be delivered to treat fungal infections.
To determine whether it remained effective at killing fungi, the researchers also tested the conjugate against four clinically important species of Candida fungi. Although more of the conjugate was needed to fully stall fungal growth compared with AmB alone, the conjugate still worked in all cases.
The higher level needed with the conjugate “is unlikely to be a problem,” says Paul B. Savage of Brigham Young University. It is still in the range where you would view the compound as potentially clinically useful, he says. However, the molecule still needs to prove effective in animal models, he says, to see if the lab results translate into better activity or diminished side effects.



Join the conversation
Contact the reporter
Submit a Letter to the Editor for publication
Engage with us on Twitter