Advertisement
Grab your lab coat. Let's get started
Welcome!
Welcome!
Create an account below to get 6 C&EN articles per month, receive newsletters and more - all free.
It seems this is your first time logging in online. Please enter the following information to continue.
As an ACS member you automatically get access to this site. All we need is few more details to create your reading experience.
Not you? Sign in with a different account.
Not you? Sign in with a different account.
ERROR 1
ERROR 1
ERROR 2
ERROR 2
ERROR 2
ERROR 2
ERROR 2
Password and Confirm password must match.
If you have an ACS member number, please enter it here so we can link this account to your membership. (optional)
ERROR 2
ACS values your privacy. By submitting your information, you are gaining access to C&EN and subscribing to our weekly newsletter. We use the information you provide to make your reading experience better, and we will never sell your data to third party members.
Analytical Chemistry
Pancreatic cancer biomarker bolsters nanoparticle-based diagnostic
Speedy sensor detects vesicles released by tumors in tiny drops of blood
by Matt Davenport
February 7, 2017

Arizona State University’s Ye (Tony) Hu and his colleagues have delivered what they hope will be a double dose of good news for detecting pancreatic cancer. Pancreatic cancer is one of the leading causes of cancer deaths because it often goes undetected in early stages, according to the Mayo Clinic.
The researchers report a rapid and inexpensive nanoparticle-based diagnostic fueled, in part, by their second finding, a biomarker on the surface of vesicles released by pancreatic tumors (Nat. Biomed. Eng. 2017, DOI: 10.1038/s41551-016-0021).
As tumors develop, they release microscopic vesicles into a patient’s blood. If biosensors could isolate and identify these vesicles, researchers could potentially screen for cancer by pricking a patient’s finger and analyzing blood droplets. This would be easier and less costly than more conventional biopsies or positron emission tomography scans, Hu says.
But all cells release vesicles and determining whether those vesicles come from healthy cells or cancerous tissue has been a challenge, he explains. Now he and his colleagues have found that vesicles released by pancreatic cancer tumors overexpress a surface protein called ephrin type-A receptor 2, or EphA2.
The researchers steered their study toward EphA2 because of evidence collected by other cancer researchers and a computerized proteomic analysis. In this study, their new diagnostic tool helps solidify the protein as a biomarker of tumor-derived vesicles.
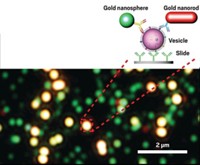
The biosensor consists of a glass slide divided into wells decorated with antibodies that capture extracellular vesicles by binding to a protein biomarker on the particles. Each well also contains gold nanorods and nanospheres that scatter light differently and shine different colors under a microscope. Nanorods appear red, whereas nanospheres glow green.
The rods are coated with antibodies specific to vesicles from pancreatic cells, and the team adorned the spheres with antibodies that bind to EphA2. Vesicles from pancreatic cancer cells thus bind both gold particle shapes. Crowding the rods and spheres onto the same vesicle causes the combo to glow yellow.
The team showed that this sensor differentiates between blood from healthy patients, patients with pancreatic cancer, and patients with pancreas inflammation. The latter condition is often confused with cancer in tests that use other biomarkers, Hu explains. The sensor requires minimal sample preparation, and its reagents are also comparable in cost to other immunoassay techniques, notably enzyme-linked immunosorbent assay or ELISA, the team reports. The sensor also works with samples as small as 1 µL, while ELISA needs more than 100 µL.
Rajesh Sardar, who develops nanosensors at Indiana University-Purdue University Indianapolis, says the new tool is exciting and transformative. “This simple, optical-based technique has the potential to screen patient samples much faster than ELISA or polymerase chain reaction,” he adds.
Pathologist Anirban Maitra agrees that the technology is promising and innovative. He works at the MD Anderson Cancer Center, as do some of Hu’s coworkers, although Maitra was not involved with the study.
Maitra, however, points out that the study was not blinded and each group was small with about 50 patients. Data in smaller studies such as this tend to look good, he says. “Validation in larger blinded sample sets becomes imperative,” he says. “I am hopeful that the PI and his team will expand their studies.”




Join the conversation
Contact the reporter
Submit a Letter to the Editor for publication
Engage with us on Twitter