Advertisement
Grab your lab coat. Let's get started
Welcome!
Welcome!
Create an account below to get 6 C&EN articles per month, receive newsletters and more - all free.
It seems this is your first time logging in online. Please enter the following information to continue.
As an ACS member you automatically get access to this site. All we need is few more details to create your reading experience.
Not you? Sign in with a different account.
Not you? Sign in with a different account.
ERROR 1
ERROR 1
ERROR 2
ERROR 2
ERROR 2
ERROR 2
ERROR 2
Password and Confirm password must match.
If you have an ACS member number, please enter it here so we can link this account to your membership. (optional)
ERROR 2
ACS values your privacy. By submitting your information, you are gaining access to C&EN and subscribing to our weekly newsletter. We use the information you provide to make your reading experience better, and we will never sell your data to third party members.
Gene Therapy
Fetal gene therapy could treat genetic diseases in the womb
Researchers are working to fix genetic conditions like Gaucher disease before birth by testing experimental therapies on fetal animals
by Ryan Cross
July 16, 2018
| A version of this story appeared in
Volume 96, Issue 30

Emboldened by recent success stories of human gene therapy trials in children and infants, researchers are now pushing to treat diseases before birth. Some scientists are excited by the idea of using fetal gene therapy to fix genetic conditions that can’t be treated after birth, but others raise questions about the technique’s feasibility and practicality in humans.
A newly published study demonstrates that surgically injecting DNA-stuffed viruses into mice can treat genetic diseases in the womb, when the potential for improvement is the most dramatic. It shows that the surgery is possible in fetal monkeys as well.
“For many genetic diseases, the damage starts early,” says Simon N. Waddington, a researcher at University College London who led the new study on an experimental gene therapy for Gaucher disease. The disease is the most common lysosomal storage disorder, a group of metabolic conditions in which an enzyme deficiency results in toxic buildup of metabolites throughout the body.
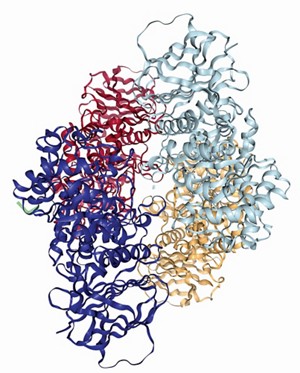
While hundreds of mutations can cause Gaucher disease, they all reduce or eliminate activity of an enzyme called glucocerebrosidase, which metabolizes glucosylceramide lipids. Doctors treat the more common Gaucher disease type 1 with biweekly injections of the missing enzyme. But the more severe type 2 variant of the disease, where the enzyme is lacking in the brain, is currently untreatable because the brain’s protective barrier prevents large enzymes from entering.
To tackle that problem, Waddington and a large team developed a virus filled with genetic instructions for making glucocerebrosidase to prevent brain degeneration in mice modeled to develop a condition resembling the type 2 disease. Since the brain damage is well under way by birth in that disease, the gene therapy was injected into the fetal mice while still in the womb.
The results, published in Nature Medicine, show that the in utero therapy treats many, but not all, aspects of the disease (Nat. Med. 2018, DOI: 10.1038/s41591-018-0106-7). Gaucher disease mice treated with the gene therapy had glucocerebrosidase activity in their brains at levels similar to those in healthy mice, but they still weighed less, had somewhat elevated brain inflammation, and didn’t perform as well on movement tests as normal mice. Still, they fared better than the untreated Gaucher mice, which were euthanized two weeks after treatment because of the severity of their disease.
Since the team used a virus able to enter the brain from the bloodstream, adeno-associated virus 9 (AAV9), Waddington also ran a test delivering a significantly higher dose of the gene therapy directly into the blood of fetal mice instead of into their brains. Mice treated this way were mostly indistinguishable from healthy mice, but because they were only allowed to live for 55 days, researchers don’t know the long-term efficacy of the intravenous injection of the therapy.
“We started this work being told that we could never make a dent in this disease,” Waddington says. Now his team is working with Apollo Therapeutics, a joint venture between three British universities and three major drug companies, to improve the therapy, develop more preclinical data, and potentially test the treatment in humans.
Advertisement
Although this isn’t the first time scientists have performed fetal gene therapy in animals, it is the most sophisticated performance of its kind. “It is really impressive. From a technical standpoint, this is bulletproof,” says W. Mark Saltzman, a professor of biomedical engineering at Yale University. Saltzman’s lab recently demonstrated the feasibility of using peptide nucleic acids to fix a mutant gene that causes β-thalassemia in fetal mice (Nat. Commun. 2018, DOI: 10.1038/s41467-018-04894-2).
Others are more skeptical about its practicality. “It is not clear how relevant this is going to be to human disease,” says Raphael Schiffmann, medical director at the Baylor Institute of Metabolic Disease in Dallas. The study’s intention is right, he says, because “once the infant is in front of you, it is too late.” The problem is that Gaucher is not commonly included in prenatal genetic tests, making the odds slim of finding many women with an affected fetus wishing to undergo the experimental therapy.
Fetal gene therapy isn’t a new idea. Researchers made the case for it in the late 1990s, the heyday of gene therapy hype right before a young man’s death during a gene therapy clinical trial stalled the field’s development for a decade.
But the concept has regained momentum as researchers make headway in developing conventional gene therapies. In December, the U.S. Food & Drug Administration approved its first gene therapy, for a rare eye disorder that can cause blindness. And recent gene therapy studies have shown promise in treating other rare diseases, including spinal muscular atrophy and Duchenne muscular dystrophy.
“It is transformative that people don’t hate gene therapy now,” Waddington says. It is enabling his group, and others worldwide, to test ideas like fetal gene therapy.
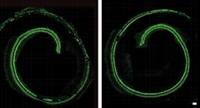
In addition to his studies in mice, Waddington teamed up with Jerry K. Y. Chan from the National University of Singapore to test the surgical procedure of delivering gene therapy to macaque fetus brains. The team was able to show that the approach worked in a larger animal by using AAV9-filled DNA encoding green fluorescent protein. “Putting a needle into the brain of a developing animal and infusing viruses is pretty heroic stuff,” Yale’s Saltzman says.
Taken in sum, Waddington’s efforts were lauded by many in the gene therapy and fetal therapy communities. “I am thrilled by the report, and I am convinced that this approach should be tested in a clinical trial,” says Holm Schneider, a professor of pediatrics at the University Hospital Erlangen in Germany.
Schneider recently led a team that treated in the womb three babies who had a rare genetic disease called ectodermal dysplasia that prevents sweat pores from developing. By injecting a therapeutic protein into the amniotic fluid, the team was able to treat the three fetuses. Thanks to the drug, their sweat glands developed normally, and no ectodermal dysplasia-related illnesses have been observed thus far in the infants, who are between one and two years old (N. Engl. J. Med. 2018, DOI: 10.1056/nejmoa1714322).
Others find the Gaucher study impressive but underscore its limitations. “The paper raises many questions,” says Neal J. Weinreb, a doctor who specializes in Gaucher at a University of Miami-affiliated clinic. One of the biggest questions, Weinreb notes, is whether the gene therapy can provide permanent, long-term production of glucocerebrosidase—critical for preventing neurodegeneration.
But Chan, who conducted the fetal gene therapy surgery in macaques, points to possible advantages to the approach. “When gene therapy is given early enough, the foreign protein may be tolerated by the fetus for life and not mount troublesome immune responses, as can be found in adult gene therapy recipients,” he says. For this reason, Chan thinks fetal gene therapy could become important for several diseases.
Chan believes the therapy “is definitely practical in humans” and says a Phase I study is the obvious next step. The group plans to develop a version that could be used in multiple types of Gaucher disease, although only fetal gene therapy could cure type 2.
Although finding enough people on which to test such a therapy could be difficult, it won’t be without precedent. University College London will soon begin what could be the first clinical trial using gene therapy in pregnant women.
Called Everrest, the trial will test a maternal gene therapy to treat a condition called fetal growth restriction, in which stalled growth of the fetus can result in stillbirth or neonatal death. By injecting a gene therapy encoding vascular endothelial growth factor into the uterine arteries of pregnant women, researchers hope to increase blood flow to the uterus and improve the growth of the developing babies.
Several other academic groups are conducting preclinical studies using in utero gene therapy and other drug modalities, such as CRISPR gene editing, to fix genetic diseases before birth. For Waddington, the growing excitement has been a long time coming.
“I stopped talking about gene therapy for a while because I was worn down by all the negative aspects,” he says. “Then gene therapy turned the corner.”



Join the conversation
Contact the reporter
Submit a Letter to the Editor for publication
Engage with us on Twitter