Advertisement
Grab your lab coat. Let's get started
Welcome!
Welcome!
Create an account below to get 6 C&EN articles per month, receive newsletters and more - all free.
It seems this is your first time logging in online. Please enter the following information to continue.
As an ACS member you automatically get access to this site. All we need is few more details to create your reading experience.
Not you? Sign in with a different account.
Not you? Sign in with a different account.
ERROR 1
ERROR 1
ERROR 2
ERROR 2
ERROR 2
ERROR 2
ERROR 2
Password and Confirm password must match.
If you have an ACS member number, please enter it here so we can link this account to your membership. (optional)
ERROR 2
ACS values your privacy. By submitting your information, you are gaining access to C&EN and subscribing to our weekly newsletter. We use the information you provide to make your reading experience better, and we will never sell your data to third party members.
Biological Chemistry
Bacteria Interfere With Painkillers
Gut microbes manipulate acetaminophen metabolism
by Sarah Everts
August 17, 2009
| A version of this story appeared in
Volume 87, Issue 33

Besides helping us digest food, the bacteria living in our gut produce chemicals that interfere with how we process the common painkiller acetaminophen. This new finding suggests that bacterial chemicals may be interfering with other drugs as well-for good or for bad.
Every person's gut has a unique assortment of trillions of microorganisms, from thousands of different species, that together produce a cornucopia of molecules in the gut, including p-cresol (C&EN, July 20, page 43). To see whether p-cresol and its metabolites could influence acetaminophen metabolism, Jeremy K. Nicholson of Imperial College London, in collaboration with scientists from Pfizer, took urine samples from humans before and after taking the painkiller (Proc. Nat. Acad. Sci. USA, DOI: 10.1073/pnas.0904489106).
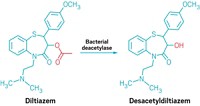
They found that the bacterial p-cresol competes with acetaminophen for O-sulfonation in the liver. The more p-cresol there is, the less acetaminophen gets sulfonated. Because sulfonation facilitates acetaminophen's excretion through the urine and thus mitigates the drug's liver toxicity, the team's results show that chemicals produced by a person's gut flora actively interfere with acetaminophen metabolism.
O-Sulfonation also helps other drugs work optimally, as in the case of minoxidil, which was originally used to treat high blood pressure and is now prescribed to counteract balding. It can also cause unwanted side effects for some medications, including the breast cancer drug tamoxifen.
"Variation in gut bacteria may therefore account for differences in the ability of the liver to metabolize certain drugs," comments Paul Watkins, director of the Institute for Drug Safety Sciences, a collaboration between the Hamner Institutes for Health Sciences and the University of North Carolina, Chapel Hill.
p-Cresol is just one gut-flora by-product, and sulfonation is just one route by which humans metabolize drugs. With trillions of bacteria in our gut, there may be many more microbial compounds that interfere with many more drug metabolism pathways, Nicholson suggests. "Assessing the effects of [gut microbe] activity should be an integral part of pharmaceutical development and personal health care," he adds.
"This study further emphasizes our need to go beyond DNA tests" to determine how an individual will respond to a drug, comments Daniel W. Nebert, who studies drug metabolism at the University of Cincinnati Medical Center. Researchers should consider other contributions to drug metabolism, such as the role of human gut bacteria and epigenetic effects.
Measurements of metabolites in urine could help predict how an individual patient—with their gut microbes—will respond to a drug, either beneficially or adversely, Watkins notes. Nicholson hopes that eventually, "gut bacteria populations might be deliberately manipulated to improve drug efficacy and to reduce adverse reactions."


Join the conversation
Contact the reporter
Submit a Letter to the Editor for publication
Engage with us on Twitter