Advertisement
Grab your lab coat. Let's get started
Welcome!
Welcome!
Create an account below to get 6 C&EN articles per month, receive newsletters and more - all free.
It seems this is your first time logging in online. Please enter the following information to continue.
As an ACS member you automatically get access to this site. All we need is few more details to create your reading experience.
Not you? Sign in with a different account.
Not you? Sign in with a different account.
ERROR 1
ERROR 1
ERROR 2
ERROR 2
ERROR 2
ERROR 2
ERROR 2
Password and Confirm password must match.
If you have an ACS member number, please enter it here so we can link this account to your membership. (optional)
ERROR 2
ACS values your privacy. By submitting your information, you are gaining access to C&EN and subscribing to our weekly newsletter. We use the information you provide to make your reading experience better, and we will never sell your data to third party members.
Drug Development
Covid-19
An emerging antiviral takes aim at COVID-19
EIDD-2801 wasn’t designed to fight the novel coronavirus, but its chemistry might make it an ideal weapon in this pandemic and the next
by Bethany Halford
May 5, 2020

As the COVID-19 pandemic shut down much of the world, George Painter’s life geared up considerably. In a matter of weeks, Painter and his collaborators have seen the antiviral they were working on—EIDD-2801—go from a promising therapeutic for influenza to a potential weapon in the fight against COVID-19, the disease caused by the novel coronavirus. The drug candidate began a human safety trial in the UK in mid-April, and a US trial is planned to begin in the next few weeks.

Painter, a virologist and chemist by training, has devoted his career to working on antivirals, coinventing several approved drugs for HIV and hepatitis B. In 2013, after decades in industry, he joined Drug Innovation Ventures at Emory (DRIVE) as its CEO and became director of the Emory Institute for Drug Development (EIDD). DRIVE and the EIDD aim to move drug candidates from early-stage development and preclinical testing to proof-of-concept clinical trials.
Painter wakes up early every morning to check in on the progress of the EIDD-2801’s clinical trial in the UK, and after a long day’s work of wrangling resources, he heads off to bed hoping that the drug candidate works as well in people as it does in animals. “You just lie awake every night worrying that you’re giving a drug to people, and you want them to be safe,” he says.
Support nonprofit science journalism
C&EN has made this story and all of its coverage of the coronavirus epidemic freely available during the outbreak to keep the public informed. To support us:
Donate Join Subscribe
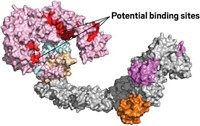
Although doctors and scientists are testing a vast arsenal of existing drugs and drug candidates in the fight against the novel coronavirus, SARS-CoV-2, EIDD-2801 stands out. It attacks the same viral enzyme, the RNA-dependent RNA polymerase, as Gilead Sciences’ remdesivir, which the US Food and Drug Administration recently granted emergency use authorization, allowing it to be used by doctors in the pandemic. But unlike remdesivir, which has to be given intravenously, EIDD-2801 can be taken orally as a pill.
This means if EIDD-2801 is shown to be safe and effective, people could take it at home rather than in a hospital. That would allow EIDD-2801 to be taken earlier in the course of the disease, killing off the virus before it wreaks havoc on the body.
EIDD-2801’s other intriguing feature is that it appears to have a high barrier to resistance. Drugs can force viruses to quickly develop mutants that aren’t affected by the drug, which then makes the drug obsolete. But EIDD-2801 hasn’t prompted that sort of resistance in lab tests despite efforts to coerce such mutants to arise.
“We always worry about resistance,” says Andy Mehle, a virologist at the University of Wisconsin–Madison. “If someone says resistance won’t emerge, they just haven’t been around viruses long enough.” But he says that sometimes viruses have to make so many changes to overcome a drug’s effect that they end up crippled as a result. Alternatively, resistance might require a simple change, but that change comes with a heavy cost to the virus’s ability to replicate. That might be the case with EIDD-2801, he says.
EIDD-2801’s story starts years before the coronavirus crisis. In 2014, Painter and his colleagues at Emory University began a project funded by the Defense Threat Reduction Agency to find an antiviral compound that could fight Venezuelan equine encephalitis virus (VEEV). During the Cold War, both the US and the Soviet Union studied VEEV as a potential biological weapon. Typically transmitted through mosquito bites, VEEV causes high fevers, headaches, and sometimes encephalitis, swelling of the brain that can be deadly.
The scientists at Emory started screening molecules, focusing specifically on nucleosides—purine or pyrimidine bases attached to a sugar that are common motifs in antiviral compounds. “We had to find something that was active, had a high barrier to resistance, and could penetrate the blood-brain barrier, because it’s an encephalitic disease,” Painter explains.
Their screening efforts turned up N-hydroxycytidine, a small molecule the Emory team dubbed EIDD-1931. “It’s a very intriguing molecule,” Painter says. “It had actually been looked at in the late 1970s by Russian and Polish scientists as a possible drug to treat smallpox infections.”
EIDD-1931 can exist in two forms. In one form, it mimics cytidine, with a single bond between the carbon and N-OH group. In its other form, which mimics uridine, it has an oxime with a double bond between the carbon and N-OH group. These two forms are known as tautomers, and the switching between them causes mismatching during transcription. So when the virus grows in the presence of EIDD-1931, its RNA-dependent RNA polymerase reads the compound as uridine instead of cytidine and therefore puts an adenosine where it should insert a guanosine. This misreading creates a massive number of mutations in the viral genome and the copied viruses can’t function.
In tests with mice infected with VEEV, EIDD-1931 was able to get into the brain and halt viral replication. And because the compound targets an enzyme that’s common to many viruses, Painter and his colleagues thought it might be able to fight more than just VEEV.
Then the researchers ran into a problem. EIDD-1931 worked well enough in mice and dogs but didn’t work in monkeys. Some sleuthing revealed that EIDD-1931’s 5'-OH was getting phosphorylated, causing the compound to get trapped in the cells that line the monkeys’ guts. It never had the opportunity to fight the virus in infected cells.
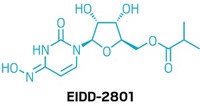
To get around this, the Emory team designed a prodrug, or a molecule that is inactive until metabolized, of EIDD-1931. Using an ester group to block the 5'-OH where phosphorylation was occurring meant enough of the molecule could reach the bloodstream, where enzymes cleave the ester and release the active form of the molecule.
“It wasn’t some major eureka moment; it was an application of a tried-and-true way to protect that 5'-OH,” Painter says. Remdesivir, for example, is also a prodrug with a blocking group at its 5'-OH. Still, he adds, because the researchers created a new chemical entity, EIDD-2801, they had to repeat many of their toxicological studies.
With hints that EIDD-2801 and its active metabolite, the triphosphate of EIDD-1931, might be able to fight other RNA viruses, Painter and his collaborators began testing it against Ebola, chikungunya, and influenza. It knocked them all out. For example, just three doses of EIDD-2801 could save ferrets (animals commonly used to study human respiratory viruses) infected with influenza from the 2009 H1N1 pandemic.
The success prompted the Emory team to reach out to researchers at Vanderbilt University and the University of North Carolina at Chapel Hill in 2015 to see if their compounds, EIDD-1931 and EIDD-2801, could fight coronaviruses. Mark Denison, who leads the Vanderbilt team studying coronaviruses and how drugs can shut them down, says his group was shocked to see that EIDD-1931 was as effective as remdesivir at fighting SARS-CoV, the coronavirus that causes severe acute respiratory syndrome, and MERS-CoV, the coronavirus that causes Middle East respiratory syndrome.
“We aren’t interested in moving forward with any compound unless it works against every coronavirus,” Denison says. EIDD-2801 passed that test.
In late 2019, Painter got a contract from the National Institute of Allergy and Infectious Diseases to move EIDD-2801 into Phase I clinical trials for influenza. The plan was to file an investigational new drug application and find a partner to help with the clinical work.
Just as the team was contemplating its next move, word of a virus spreading in Wuhan, China, was starting to make news. One of Painter’s collaborators, UNC coronavirus expert Ralph Baric, immediately alerted him that the new pathogen was probably a coronavirus—one that EIDD-2801 could potentially combat.
Denison says the research team knew a coronavirus outbreak was inevitable. “Every single one of our grants, every single one of our papers predicted that this event was going to happen that’s occurring right now,” he says. “The whole goal of our drug development was to plan for this.”
“We thought, ‘Oh my god, it’s a coronavirus. We should be ready,’ ” Painter recalls.
In early March, the research team tested EIDD-1931 in human cells infected with SARS-CoV-2. The compound was able to knock out the virus. It also effectively fought coronaviruses that are resistant to remdesivir.
The researchers sped up efforts to get EIDD-2801 into clinical studies for SARS-CoV-2. Painter says they wrote the investigational new drug application for EIDD-2801 in 48 h. The application also had the fastest turnaround—about 7 days—he’s ever seen from the US Food and Drug Administration.
In March, DRIVE licensed EIDD-2801 to Ridgeback Biotherapeutics for human studies. In April, the FDA and the UK Medicines and Healthcare Products Regulatory Agency cleared the way to begin Phase I human testing, which began April 10 in the UK. In his whistleblower complaint, Rick Bright, who was removed as head of the US Biomedical Advanced Research and Development Authority (BARDA) in April, asserts that Ridgeback pressured BARDA to provide funding to manufacture EIDD-2801 despite Bright's concerns that similar drugs in its class have mutagenic properties.
Virologists are encouraged by EIDD-2801's performance in published reports. Juliet Morrison, a virologist at the University of California, Riverside, says the compound appears promising from its success in cell culture studies and experiments in mice with SARS-CoV and MERS-CoV. To have an impact, it will need to be given early, she says, before the virus has had time to harm the body. EIDD-2801 “would probably not be useful for the later stages of the disease but would be useful for disease prevention potentially,” she says.
Painter says that ideally, EIDD-2801 would be given once someone has been exposed to SARS-CoV-2—to prevent infection—or up to a week or so after someone has been infected.
“We have published over and over again that if these drugs are given late, they don’t work,” Denison says of his work with remdesivir and EIDD-2801. They kill the virus no matter when you give them, but he says it’s as if your arm catches on fire: “Someone can come along with a fire extinguisher and put it out, but that’s not going to treat your arm. If the damage is done, the damage is done.”
The fact the EIDD-2801 can potentially be active against a broad range of viruses is a rarity, says Dennis C. Liotta, inventor of several key HIV drugs and executive director of the EIDD. “Almost no antiviral agent is active against multiple viruses,” he says. “Most of our drugs are what we call ‘one bug one drug’ compounds.”
That broad activity is important when you’re preparing for pandemics, Liotta says. “Once you demonstrate its safety and efficacy, you’d like to build up a big supply of it so that when the next pandemic comes along, you have something you can potentially try with people, and if it works, you can stop that viral pandemic in its tracks.” Even if it doesn’t work, he adds, at least you’d have something in your arsenal, which we don’t really have now.
Before this outbreak, “a lot of people said, ‘Who cares about coronaviruses?’ ” Liotta says. They “weren’t given the kind of priority that, clearly now, the situation suggests they deserve.” The coronavirus crisis, he says, should be a wake-up call to funding agencies around the world to rethink their priorities. “It’s a terrible way to have to do that. But I do think that we were ahead of the curve, and we need a lot of people to be ahead of the curve, because no one has a monopoly on how to make effective drugs.”
UPDATE
This story was updated on May 19, 2020, with clinical trial information for EIDD-2801 in the US and to include information in the whistleblower complaint filed by Rick Bright, who was removed as head of the US Biomedical Advanced Research and Development Authority (BARDA) in April.



Join the conversation
Contact the reporter
Submit a Letter to the Editor for publication
Engage with us on Twitter