Advertisement
Grab your lab coat. Let's get started
Welcome!
Welcome!
Create an account below to get 6 C&EN articles per month, receive newsletters and more - all free.
It seems this is your first time logging in online. Please enter the following information to continue.
As an ACS member you automatically get access to this site. All we need is few more details to create your reading experience.
Not you? Sign in with a different account.
Not you? Sign in with a different account.
ERROR 1
ERROR 1
ERROR 2
ERROR 2
ERROR 2
ERROR 2
ERROR 2
Password and Confirm password must match.
If you have an ACS member number, please enter it here so we can link this account to your membership. (optional)
ERROR 2
ACS values your privacy. By submitting your information, you are gaining access to C&EN and subscribing to our weekly newsletter. We use the information you provide to make your reading experience better, and we will never sell your data to third party members.
Biological Chemistry
Getting To The Root Of Cancer
The dark side of stem cells is initiating a revolution in cancer research
by Sarah Everts
January 15, 2007
| A version of this story appeared in
Volume 85, Issue 3
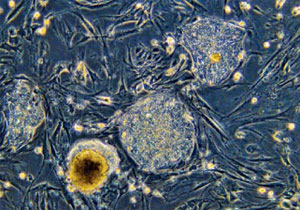
COVER STORY
Getting To The Root Of Cancer
If you catalog the characteristic features of a cancer cell, they sound uncomfortably similar to those of a stem cell. Both cancer and stem cells boast a seemingly magical ability to grow perpetually, and both exhibit immunity to internal switches that initiate cell suicide.
The similarities were certainly not lost on stem cell scientists. As early as the 1950s, researchers were suggesting a link between stem cells and cancer, but the technology to prove it was decades in coming.
The cancer stem cell theory argues that not all cells in a tumor are created equal. Only a small subset—one cell in a million for leukemia—has the capacity to proliferate and differentiate into all of the cells that form a tumor. These cells, known as cancer stem cells, are increasingly considered the root of all cancer.
"A stem cell is a stem cell, irrespective of whether it's making a normal organ or a tumor," says Craig T. Jordan, a stem cell researcher and professor of medicine at the University of Rochester, in New York. "That's the common tie that people had not realized earlier or at least had not been able to study."
The means to do so materialized in the early 1990s, when advanced cell-sorting technology allowed John E. Dick and his colleagues at the University of Toronto to isolate a single blood cancer stem cell. These cells could generate entire leukemias in mice, while other malignant cells could not.
The implications of this discovery on cancer research are weighty. What if irradiation and chemotherapies shrink tumors but don't kill the cancer stem cells that generated them? Could this be the cause of cancer recurrence? Even worse, could such treatments create more cancer stem cells from normal stem cells?
Although Dick's finding caused a ripple in the stem cell world, the discovery didn't resonate in other disciplines immediately. "The stem cell field was still fairly small, so the discovery was not talked about much elsewhere," Dick says. Cancer research was focused at the time on the physiology of entire tumors, like their ability to create complex blood vessel circuitry. To boot, blood is a weird liquid organ, and some thought the finding might not represent something general about cancer.
A "revolution," Dick says, happened in 2003, when other groups began isolating cancer stem cells from solid tumors. A breast cancer stem cell was characterized by Michael F. Clarke's group at the University of Michigan, Ann Arbor; he is now at Stanford University. The trick was identifying a cell-surface protein unique to breast cancer stem cells and then showing that cells with that marker could re-create a cancer. Then a few months later came a brain cancer stem cell, reported by Peter Dirks' group, also at the University of Toronto.
"By this time, the research community was better informed about stem cells," Dick says. "People who didn't work in stem cell biology could read the papers and understand the implications." Despite the advent of better chemotherapy drugs, cancer research has made only an incremental advance in long-term survival of cancer patients, he adds. "People were thinking that perhaps the cancer paradigm needed to change."
And so it has. Stem cells are now being widely investigated as key players in a variety of cancers, including colon, bone, cervical, lung, and prostate.
Evidence suggests that eradicating such cancer stem cells may require weapons different from those in the current arsenal. Last November, a landmark paper showed that stem-cell-like tumor cells with a signature protein called CD133 are actually more resistant to radiation than other glioblastoma (brain) cancer cells (Nature 2006, 444, 756).
Radiation doesn't cause less DNA damage in cancer stem cells than in other tumor cells. Instead, the cancer stem cells simply do a better repair job. "The implication of these results is that radiation treatment fails in the long run because it cannot kill the subpopulation of CD133+ tumor-initiating cells," Dirks comments. Patient treatment outcomes back this conclusion. Radiation therapy has been the predominant treatment for glioblastoma for 40 years, killing tumor cells in the short term but failing to provide a long-term cure for the cancer.
And therein lies a terrible truth. Currently, clinical trials for new chemotherapeutics look for end points such as tumor reduction, but they do not determine whether the therapy eradicates cancer stem cells.
"For cancer therapy to take a step forward, you have to develop drugs where you are considering cancer stem cells in the drug development process, and that essentially has never happened," Jordan tells C&EN. Many cancer stem cell assays are extremely new, or in development, and they are not yet widely used. He says "we have to design our clinical end points more intelligently so that we can actually assess whether the drug is successful at the level of the tumor stem cell."
Jordan points to the drug Gleevec. It's a treatment for chronic myelogenous leukemia, with few if any side effects. "Gleevec is a phenomenal success story and has revolutionized the way cancer is treated," Jordan says. "However, what's become apparent in recent years is that the drug kills everything but the stem cell. As soon as the cells emerge from the stem cell, they are killed by the drug if you take it every day."
Fortunately, the drug has a low toxicity, Jordan says. "It keeps the disease suppressed. But patients that are on it will likely have to stay on it forever. There's a cancer root that does not go away."
So what to do? One strategy is to compare cancer stem cells and normal stem cells to identify molecular targets unique to cancer stem cells, says Mickie Bhatia, director of the McMaster Stem Cell & Cancer Research Institute in Hamilton, Ontario. But it remains difficult to isolate the cancer stem cell's healthy counterpart, making it tough to identify distinguishing features of the cancer stem cell and thus to find drugs that specifically target it and not the normal stem cell.
A rare success was reported in 2005 when the first small molecule to target cancer stem cells was discovered (Blood 2005, 105, 4163). Parthenolide, a natural product isolated from a medicinal plant known as feverfew, induces apoptosis in leukemia stem cells.
Parthenolide is an inhibitor of a protein called NFKB, says Jordan, whose group made the discovery. NFKB is part of a protein complex that turns on genes associated with proliferation and growth. But NFKB inhibition alone cannot kill leukemia stem cells, Jordan notes. Parthenolide's secret is that it is not only an NFKB inhibitor but also a strong inducer of oxidative stress. These seem to be the two molecular signals that allow the compound to selectively kill leukemia stem cells but not their healthy counterparts, he says.
Another strategy to selectively disarm cancer stem cells is to induce them to differentiate, thereby taking away their ability to form a suite of malignant cells. Scientists at the Stem Cell Research Institute in Milan, Italy, recently published a study that showed that exposing brain tumor stem cells to a protein that induces differentiation in normal stem cells incites cancer stem cells to follow suit (Nature 2006, 444, 761). Differentiation severely limits the cancer stem cells' ability to form new tumors, they found.
Other researchers are trying to figure out if cancer stem cells can be neutralized by modulating the proteins that block or encourage transcription of genes involved in differentiation.
Although strategies to kill cancer stem cells are on the rise, scientists are still struggling to figure out exactly what generates these malignant cell factories in the first place. When a normal stem cell divides, it usually splits into another stem cell and a progenitor cell that can differentiate into a more mature cell. Some researchers wonder if progenitor cells suffer DNA mutations or chemical modifications that reprogram them into cancer stem cells. Others believe cancerous stem cells arise through malignant transformation of normal stem cells.
Two papers coming out in the February issue of Nature Genetics provide evidence for the latter theory. Peter W. Laird at the University of Southern California and his colleagues reveal that some healthy stem cells can be "locked" into a state that predisposes them to malignancy, supporting the notion that cancer stem cells come from normal stem cells. Even as the exact origins of cancer stem cells are being ironed out, their importance in cancer has already taken hold.



Join the conversation
Contact the reporter
Submit a Letter to the Editor for publication
Engage with us on Twitter