Advertisement
Grab your lab coat. Let's get started
Welcome!
Welcome!
Create an account below to get 6 C&EN articles per month, receive newsletters and more - all free.
It seems this is your first time logging in online. Please enter the following information to continue.
As an ACS member you automatically get access to this site. All we need is few more details to create your reading experience.
Not you? Sign in with a different account.
Not you? Sign in with a different account.
ERROR 1
ERROR 1
ERROR 2
ERROR 2
ERROR 2
ERROR 2
ERROR 2
Password and Confirm password must match.
If you have an ACS member number, please enter it here so we can link this account to your membership. (optional)
ERROR 2
ACS values your privacy. By submitting your information, you are gaining access to C&EN and subscribing to our weekly newsletter. We use the information you provide to make your reading experience better, and we will never sell your data to third party members.
Oncology
Clinical data buoys protein degradation field
Early peek at two trials at ASCO gave signal for how a new class of drugs might perform
by Asher Mullard, special to C&EN
May 29, 2020

Small molecules that drive the breakdown of their protein targets, rather than just inhibiting them, have been capturing the imagination of drug hunters for the better part of a decade. Clinical data from Arvinas and Bristol-Myers Squibb (BMS), presented today at the American Society of Clinical Oncology (ASCO) annual meeting, which was in a virtual format, is now further fueling the dream. Early studies showed that these drugs, called protein degraders, can be safe in humans, drive target degradation and provide hints of therapeutic efficacy.
“This is really going to provide a lot of confidence for people in academia and in industry to continue to push for this new paradigm,” says Shaomeng Wang, a medicinal chemist at the University of Michigan who has discovered multiple targeted degraders. Wang was not involved in either study.
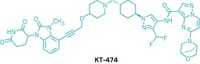
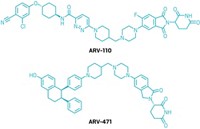
Arvinas’s ARV-110 is the prototypical targeted degrader. A bifunctional small molecule, it uses one arm to bind the androgen receptor (AR), a prostate cancer target, and the other to tether to an E3 ligase. The E3 ligase then tags the AR with ubiquitin, marking it for degradation by the cell’s proteasomal recycling system. The newly released ASCO data highlight results from the first 22 patients from a safety and efficacy trial that was launched in March 2019.
On the safety side, treatment was generally well-tolerated, says Arvinas chief medical officer Ron Peck. There were worrying increases in liver enzyme levels in 2 patients, but the Arvinas team ultimately traced both signals back to a problematic interaction between ARV-110 and the lipid-lowering drug rosuvastatin. The first patient suffered renal failure. When the second stopped taking rosuvastatin, his liver enzyme levels normalized and he was able to resume ARV-110 therapy.
“We don’t suspect that this is going to be a class effect,” says Peck. “I would be in a different mood if we couldn’t have found an explanation for those events.” The company is still increasing the dosing of the drug to find its toxicity ceiling.
The study also hints at efficacy, although only in a narrow subset of patients. The AR can pick up various mutations and abnormalities during the course of disease, and only some of these are susceptible to ARV-110-induced degradation. When Arvinas used circulating tumor DNA to zoom in on patients with these degradable forms of AR, they found that 2 out of 7 patients experienced marked declines in the prostate cancer biomarker PSA. These patients both had the same two point mutations — called H875Y and T878A — in their AR. They experienced PSA declines of 74% and 97%, and their tumors remained stable after 30 weeks and 18 weeks on treatment, respectively, at the data cut-off.
“We’re obviously extremely excited that at this stage we’re already seeing anti-tumor activity,” says Peck.
Arvinas saw preliminary evidence of AR-degradation in a tumor tissue biopsy from 1 patient, but it is not disclosing the depth of degradation until it has biopsy data from more patients in hand.
Wang is encouraged by the results. The safety profile generally looks good and the rosuvastatin signal is most likely only a problem for ARV-110, rather than for the whole modality, he agrees. The efficacy signal could have been better, he argues, but higher dosing could yet unlock more activity. “Overall, this is positive,” says Wang. His team has developed an AR-targeted degrader as well, which it has licensed to Oncopia Therapeutics.
BMS’s designed targeted degrader approach, meanwhile, builds on insights gained through its $74 billion acquisition of Celgene, and its prize jewels, the blood cancer treatments lenalidomide and pomalidomide. Researchers didn’t initially understand how these imide drugs kill cancer cells, but subsequently discovered these agents also drive targeted degradation. By binding the E3 ligase Cereblon, they improve the ability of the E3 ligase to then recruit and tag transcription factors Ikaros and Aiolos for disposal.
Researchers have since been working to deliberately design new versions of these molecular glues. The most advanced resulting compound, CC-92480, is particularly good at breaking down the protein targets, the team reported earlier this year in the Journal of Medicinal Chemistry. “What we showed was the deeper the degradation of Aiolos, the more rapid the induction of cell death in a myeloma cell line,” adds Kristen Hege, senior vice president of early clinical development in hematology, oncology, and cell therapy at BMS.
First data from a Phase I study of CC-92480 in combination with the corticosteroid dexamethasone in multiple myeloma looks promising. In a cohort of 11 patients whose disease had progressed with other treatments and who received the favored dosing regimen, 55% of patients saw their cancers shrink by at least 50%. At this dose, CC-92480 depleted Aiolos levels by 93% from baseline within just 3 hours of treatment.
“Conceptually, you have to say, ‘Wow there’s great potential here’,” says Hege. BMS now counts targeted degradation as a core area of discovery and translational research, she adds, with applications in cancer and beyond. For the company’s next targeted degrader act, it is pivoting to a bifunctional small molecule, with an AR-targeted program of its own.
Wang hopes that interest in molecular glue degraders stays strong, however, because these smaller molecules may offer more ‘drug-like’ properties than the bulkier bifunctional degraders. “If we can find more drugs that function like these molecular glues, I think that will be the next frontier in drug discovery,” says Wang.
These clinical results buttress the growing list of big pharma and start-up firms working on targeted degraders. Roche partnered with Vividion Therapeutics in a $135 million targeted degradation deal last week. Monte Rosa Therapeutics launched this week, with $32.5 million in backing.
UPDATE
Due to an error in the company's data, this story was updated on May 29, 2020, to correct the percentage of PSA declines in the Arvinas trial. One of the patients experienced a decline of 97%, not 94%.



Join the conversation
Contact the reporter
Submit a Letter to the Editor for publication
Engage with us on Twitter